No mother wants their kid hospitalized, but years ago diabetes almost took Katie Chaney’s now 7-year-old, Beckett’s life.
Beckett was diagnosed when he was only fifteen months.
“It was one of those moments where you sort of feel like the whole world crashes down around you,” Chaney said.
Beckett’s blood sugar was 680 at the time of his diagnosis. He was very sick, as he suffered from undiagnosed type one diabetes. Although, his urgent diagnosis was helpful.
“About six months after that, Mason was diagnosed with type one diabetes when he was eight,” Chaney said.

Now the Chaney household has two diabetic children living under one roof. Chaney said this was abnormal for them.
“We don’t have any family history of type one diabetes, so it was a big surprise and shock to our family” Chaney said.
Type One diabetes means both of her sons’ immune systems attack healthy cells in the pancreas.
“It felt impossible,” said Chaney.
Suddenly this mom needed a crash course in pediatric endocrinology. She said she had to “get up to speed on how the human pancreas functions and try to mimic that.”
Now looking at Beckett, he’s a normal seven-year-old, and Mason is a typical thirteen-year-old.
“When you first get diagnosed with it, you just can’t really believe it and you don’t want it to be happening,” Mason said. “It just is what it is," said Beckett.
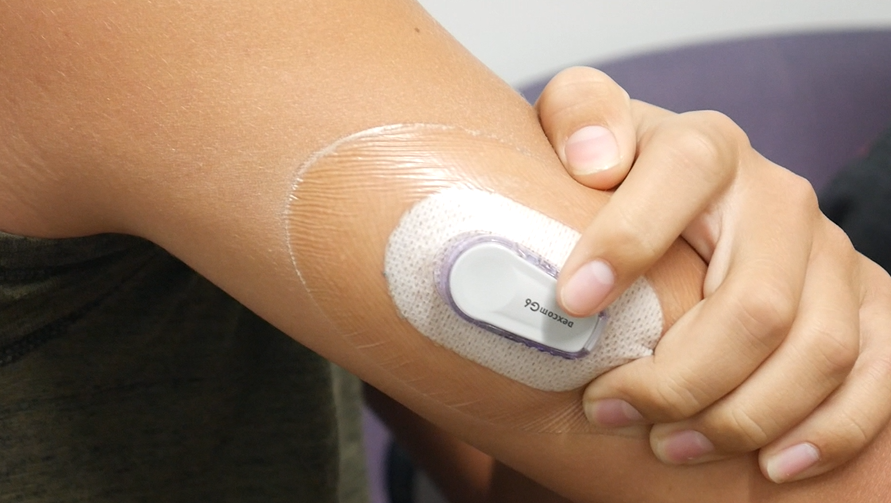
Now for the past year, the brothers have managed juvenile diabetes with the help of the latest technology. The FDA calls it an “artificial pancreas device system”. A sensor under the skin automatically measures blood sugar levels. The readings are sent to a pump. The device calculates the amount of insulin required.
WRTV Anchor, Megan Shinn asked “do you feel like it’s pretty easy?"
Beckett tells Megan, “uh, yeah, sometimes”.
The children must input what they eat at times, to help calculate the amount of insulin they need. So, it doesn’t completely work on its own but the devices do communicate with each other independently.
Doctor Tamara Hannon is the medical director for the pediatric diabetes clinic at Riley and she calls it a “closed loop system”. She’s also both boys’ pediatric endocrinologist. ,
“They did great before, but they are excellent,” Hannon said.
Doctor Hannon said the technology is a huge game changer. She said one of every 350 school aged child has type one diabetes. So pretty much every school has students with the diseases.
The formal name for what the kids have is the Omnipod Five.

“I’ve been doing this for you know, twenty some years, ”Doctor Hanon said. “Over the past three years, I would say I’ve seen more people achieve target blood sugars because of the overnight automation of blood sugars.”
Hannon explains that overnight is the scariest time because children might not notice a dangerous blood sugar change. Insulin levels automatically adjust at night, and no one wakes up for shots.
She said most importantly, it’s helping these kids… be kids. “To get tight control is hard with kids especially as young as they are and as active and they’re growing, and they’re eating and want to do all the things that kids do,” Doctor Hannon said.
“In my opinion it helps them be kids first and it lets diabetes kind of fall into the background of their lives, which is where I would like it go be,” said Chaney .
Chaney said the “Omnipod 5” costs them about three hundred dollars a month with insurance. Beckett and Mason still must visit Riley every three months for checkups.
Riley does a three-day training on diabetes education before they let parents or caregivers go home. For more info from Riley, click on this link.
According to the US Census Bureau, diabetes affects about 37,000,000 Americans, including adults and youth. It’s important to understand Type One diabetes. First, it doesn’t mean kids can’t have sugar and kids won’t grow out of it.
The signs and symptoms of type one diabetes in children include increased thirst, frequent urination, increased hunger, fatigue, and blurry vision among other symptoms.
As a reminder, there is a difference between type one and type two diabetes.








